2019 Volume No 38 – pages 63-78
Title: Biology of soft tissue repair: gingival epithelium in wound healing and attachment to the tooth and abutment surface |
Authors: S Gibbs, S Roffel, M Meyer, A Gasser |
Address: Department of Molecular Cell Biology and Immunology, O/2 building room 11E05, VU University Medical Centre, Amsterdam UMC, Amsterdam, the Netherlands. |
E-mail: s.gibbs at acta.nl |
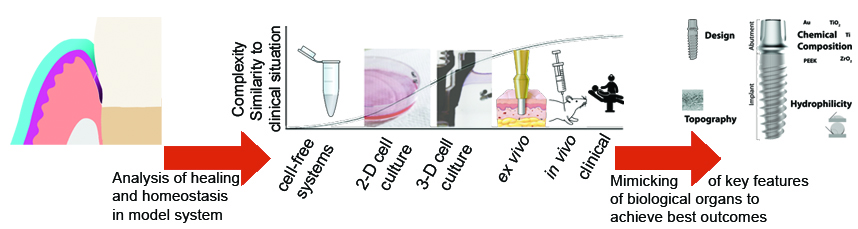
Abstract: Epithelium attachment to the tooth or abutment surface is necessary to form a biological seal preventing pathogens and irritants from penetrating the body and reaching the underlying soft tissues and bone, which in turn can lead to inflammation and subsequent bone resorption. The present review investigated oral wound closure and the role of micro-environment, saliva, crevicular fluid and microbiota in wound healing. The importance of the junctional epithelium (peri-implant epithelium) attachment to the abutment surface was investigated. Current research focuses on macro-design, surface-topography, surface-chemistry, materials, coatings and wettability to enhance attachment, since these optimised surface properties are expected to promote keratinocyte attachment and spreading through hemi-desmosome formation. Detailed studies describing the extent of junctional epithelium attachment – e.g. barrier function, hemi-desmosomes, epithelium quality, composition of the external basement membrane or ability of the epithelium to resist microbial penetration and colonisation – are not yet reported in animals due to ethical considerations, scalability, expense, technical challenges and limited availability of antibodies. In vitro studies generally include relatively simple 2D culture models, which lack the complexity required to draw relevant conclusions. Additionally, human organotypic 3D mucosa models are being developed. The present review concluded that more research using these organotypic mucosa models may identify relevant parameters involved in soft-tissue-abutment interactions, which could be used to study different macro-shapes and surface modifications. Such studies would bridge the gap between clinical, animal and traditional in vitro cell culture studies supporting development of abutments aiming at improved clinical performance. |
Key Words: Oral epithelium, junctional epithelium, abutment, implant, attachment, biological seal, surface, basement membrane, saliva, crevicular fluid. |
Publication date: August 14th 2019 |
Article download: Pages
63-78 (PDF file) |